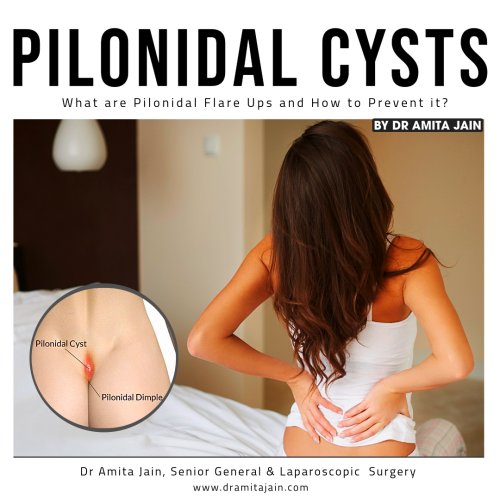
A pilonidal flare-up is a painful swelling or infection that occurs near the tailbone, usually at the top of the buttocks crease. It is caused by a pilonidal cyst, which forms when hair, sweat, and dead skin cells become trapped under the skin. These cysts can become infected, leading to pus buildup, redness, and severe pain. Pilonidal disease is more common in young adults, especially men, people with thick body hair, or those who sit for long periods.
While flare-ups can be extremely uncomfortable, the good news is that with proper hygiene and preventive care, they can be managed and often avoided altogether, says Dr Amita Jain, who is a senior general and laparoscopic surgeon and one of the leading doctors for pilonidal sinus treatment in Delhi and India.
What Is a Pilonidal Flare-Up?
A pilonidal flare-up happens when a cyst or sinus in the cleft between the buttocks becomes inflamed or infected. The trapped hair and debris act as a foreign body, causing the immune system to react. This results in redness, swelling, tenderness, and sometimes pus discharge. The pain can make sitting or walking difficult. In some cases, an abscess (a pocket of infection) forms, which may need to be drained by a doctor. Common symptoms include:
- A painful lump near the tailbone
- Redness or swelling in the lower back area
- Pus or blood discharge
- Foul odor from the infected area
- Fever or fatigue in severe cases
Flare-ups can occur suddenly, especially after long sitting hours, sweating, or friction caused by tight clothing.
What are Some of the Common Causes of Pilonidal Flare-Ups?
Several factors contribute to pilonidal flare-ups:
- Poor hygiene: Sweat and dirt accumulation can irritate the skin and promote bacterial growth.
- Ingrown hair: Hair growing back into the skin can trigger inflammation.
- Prolonged sitting: People with sedentary jobs or long driving hours are more prone to pressure and friction in the tailbone area.
- Tight clothing: Clothes that rub against the skin increase irritation and trap sweat.
- Obesity: Excess body weight deepens the buttock crease, increasing sweat and friction.
- Family history: Some people may have a genetic tendency toward pilonidal cysts due to skin structure or hair type.
How to Prevent Pilonidal Flare-Ups?
While pilonidal cysts can recur, consistent preventive care can significantly reduce flare-ups.
- Maintain Good Hygiene: Keep the tailbone area clean and dry. Shower daily and gently exfoliate to prevent the buildup of hair and dead skin cells. Use mild soap and warm water to cleanse the area.
- Remove Excess Hair: Regular hair removal—through shaving, depilatory creams, or laser treatment—helps prevent hair from burrowing under the skin. Always use clean tools and avoid harsh shaving methods that can irritate.
- Avoid Prolonged Sitting: Take short breaks if your job involves long sitting hours. Stand, stretch, or walk every 30–60 minutes to reduce pressure on the tailbone.
- Wear Loose, Breathable Clothing: Choose cotton or moisture-wicking fabrics to prevent sweat buildup. Avoid tight jeans or synthetic materials that trap heat and friction.
- Maintain a Healthy Weight: Reducing excess body fat lessens the depth of the buttock crease and minimises friction. A balanced diet and regular exercise help maintain a healthy body weight and skin condition.
- Treat Early Signs Promptly: At the first sign of pain or swelling, apply a warm compress to ease discomfort and improve blood flow. Avoid squeezing or attempting to drain the cyst yourself. If symptoms persist, consult a doctor to prevent the infection from worsening.
Pilonidal flare-ups can be painful and disruptive, but they are largely preventable with simple lifestyle adjustments and good hygiene habits. Understanding the causes and taking proactive measures—like keeping the area clean, minimising friction, and managing body hair—can go a long way in avoiding recurrent infections. For those who experience frequent or severe flare-ups, medical treatments, including minor surgery, may offer long-term relief. Ultimately, caring for your skin and maintaining healthy daily habits is the best defence against pilonidal flare-ups.

Dr Amita Jain, one of the most experienced General and Laparoscopic Surgeons in Delhi, is widely recognised for her expertise in hernia, piles, gallbladder, fissure, and fistula surgeries. With an outstanding career spanning over 29 years, Dr Amita Jain has earned her place among the top General and Laparoscopic surgeons in Delhi and India, known for her precision, compassion, and consistent surgical excellence. She was the Professor of Surgery at the Army College of Medical Sciences and Base Hospital, Delhi Cantt. In 1994, she was commissioned as a surgeon under the United Nations Mission in Congo.
Dr Amita Jain currently serves as the Senior General and Laparoscopic Surgeon at Fortis C-DOC Hospital, B-16, Chirag Enclave, Opposite Devika Tower, Greater Kailash 1, New Delhi, Delhi 110048. She is also the Head of Department, Laparoscopic and Trauma Surgery at Artemis Lite Hospital (Delhi), Senior General and Laparoscopic Surgeon at Rosewalk – Luxury Maternity Hospital in Delhi and Rainbow Children Hospitals (at Malviya Nagar and Panchsheel Park, New Delhi)
Dr Amita Jain has successfully performed a wide range of complex general surgeries, including both open and minimally invasive procedures, with a strong focus on trauma care, onco-surgical techniques, and reconstructive surgeries. Her medical specialisation includes – Gallbladder surgeries, appendix removal surgeries, hernia repair surgeries, Pilonidal Sinus treatments, varicose vein and piles surgeries, fistula surgeries and fissure surgeries. Learn More about Dr Amita Jain.
Dr Amita Jain has also authored some of the key medical journals and publications, like ResearchGate, IJSR
Note: the articles are written with Dr Amita Jain’s professional insights and referring to her medical publications.